 /arc-anglerfish-arc2-prod-dmn.s3.amazonaws.com/public/XW5ZS7ECDIGHTWR7MUHRGAHI3A.png)
In the INVEST trial with more robust sample size, criticisms include a high crossover rate, low pain score required for enrollment, lack of MRI for enrolled patients, as well as similar criticisms to the study by Buchbinder et al. In the first trial by Buchbinder et al, criticisms include a small sample size of 78 patients, a high proportion of subacute and chronic VCF, and a perceived small volume of injected cement. The original negative randomized controlled trials comparing vertebroplasty to sham procedures were published in 2009. Within these practice parameters, the complication rate from vertebral body augmentation is <1% for osteoporotic VCF and <5% for malignant VCF.Ĭlinical success rate defined as improvement in pain, disability, or quality of life is 80 to 98% for osteoporotic VCF and 70 to 92% for malignant VCF.Īny discussion of vertebral body augmentation must acknowledge the conflicting evidence supporting its use. Relative contraindications include nerve or cord compression. However, delaying intervention may lead to more modest benefits from vertebral body augmentation.Ībsolute contraindications include infection, whether systemic or local, as well as uncorrectable coagulopathy, and allergy to PMMA. The trial of nonoperative management is traditionally 6 weeks corresponding to the natural history of disease and inclusion criteria for clinical trials. 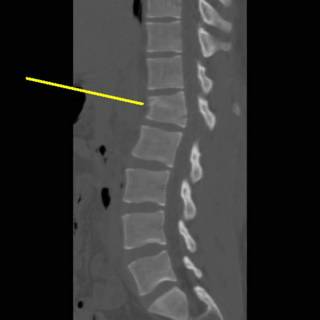
The most common indication for vertebroplasty and kyphoplasty is symptomatic VCF refractory to nonoperative management. The AOSpine classification system facilitates consistent image interpretation between providers. Multiple classification systems for vertebral body fractures exist, but one commonly utilized system is the AOSpine classification which dichotomizes fractures into those that violate the endplates (e.g., wedge or split fractures) or posterior cortex (e.g., burst fractures). Infrequently, comparison radiographs or computed tomography (CT) demonstrating an interval fracture correlating with acute symptoms can be sufficient. In patients with a contraindication to MRI, a bone scan can be performed with or without single photon emission computed tomography (SPECT) for more precise localization. MRI with gadolinium can be used to evaluate for malignancy. Additional benefits of MRI include finding additional acute VCF which may be occult on radiographs, and evaluating for additional etiologies of back pain. MRI permits localization of the afflicted vertebral body, defines the fracture clefts, and triages patients to nonoperative management or vertebral body augmentation. Preprocedural magnetic resonance imaging (MRI) is preferred to document bone marrow edema on short tau inversion recovery (STIR) sequence. The Society of Interventional Radiology (SIR) recommends platelets of at least 50,000 and international normalized ratio (INR) of at most 1.5.Īntiplatelets and anticoagulants should be held according to SIR guidelines for high-risk procedures. Patients should have laboratories drawn to check for coagulopathy. It can be helpful to further evaluate patients with a validated survey to determine pain severity (Roland–Morris Back Pain score), quality of life (the Short Form 36 Health Survey), or disability (Oswestry Disability Index). Kyphosis may result in decreased respiratory capacity.Įxtremity numbness or weakness suggests nerve impingement of different etiologies, which may benefit from alternative therapy such as epidural steroid injection. On physical exam, the patient will have focal midline or paramidline tenderness with firm palpation. It is important to determine whether there are symptoms of spinal cord compression, such as bowel or bladder dysfunction, to properly triage these patients to neurosurgical evaluation. Radicular symptoms are atypical and should warrant evaluation for nerve compression or spinal stenosis. Typical pain descriptors are midline pain localized to a specific spinal level with a band-like distribution that is worse with movement or weight bearing. In those with chronic back pain, patients frequently point to a specific day that their symptoms worsened which may indicate an acute VCF. 
The initial patient history should include the onset of symptoms, quality and severity of pain, and exacerbating factors. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
